Obesity, and other health related issues are a major and growing concern for employers and many don’t know how to deal with these concerns proactively and effectively. Obesity seems to be the elephant in the room (poor choice of words – sorry) in terms of risk and safety and hitherto mostly dealt with in relation to health. I haven’t had much to do with the issue except hearing stories of obesity caused by FIFO lifestyle. I hear it raised a lot “unofficially” as a contributor to incidents or the severity of injuries. I have no doubt it is the also cause of much bias at many stages of employment cycle. I had a business owner tell me recently that they would never employ a smoker and I am sure many employers have the same biases toward those who are obese, even if they will not admit it, or even consciously be aware of it? Here is an interesting article sent to me by Shelby Schneid – a student and OHS intern working for Siemens. He raises some good starting points and could lead to some interesting discussion ?
Organizational Behavior’s Link with Obesity
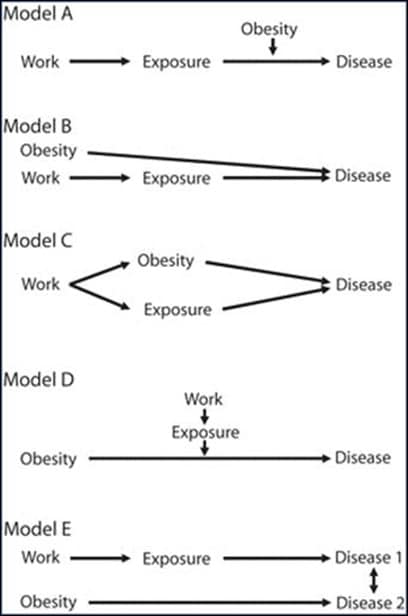 Obesity in the workplace is becoming more relevant as the obesity epidemic continues to grow in the United States. Due to the rising epidemic, obesity is becoming a factor in organizational behavior. According to Centers for Disease Control and Prevention (CDC), more than one-third of U.S. adults are obese. Obesity increases the change of heart disease, stroke, type two diabetes and cancer. The figure to the right shows the interrelationships of work, obesity, and disease.
Obesity in the workplace is becoming more relevant as the obesity epidemic continues to grow in the United States. Due to the rising epidemic, obesity is becoming a factor in organizational behavior. According to Centers for Disease Control and Prevention (CDC), more than one-third of U.S. adults are obese. Obesity increases the change of heart disease, stroke, type two diabetes and cancer. The figure to the right shows the interrelationships of work, obesity, and disease.
Model A, a workplace exposure leads to an occupational disease. This relationship may be modified by weight gain or obesity, causing the risk to be greater. Model B shows 2 independent pathways to disease, obesity being one and workplace exposure another. Model C shows a combination of both models A and B, with work as the source of the adverse environmental exposures as well as a contributor to obesity, and the combination or each factor independently resulting in modified disease risk. Model D shows how workplace exposure may be an effect modifier of an obesity-disease relationship. Finally, Model E shows how obesity may cause a particular disease and workplace exposure may cause another disease. In other words, having one disease may put a worker at increased risk of the other.
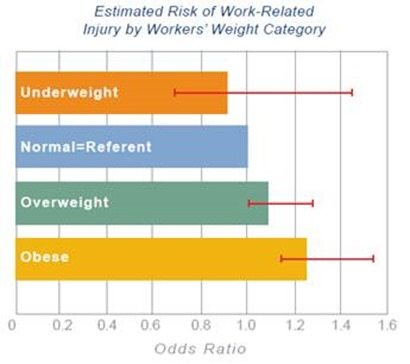
Studies have shown that obesity was associated with a 25 percent higher risk of work-related injury, independent of all other relevant factors, such as age, work hours and occupational hazards. In our field of work, damage resulting in obesity or obesity-related changes in physiology may compromise muscular, neural, and vascular tissues, making them more susceptible to a vibration or repetitive movement induced injury.
 In our field of wind energy, personal protective equipment (PPE) has a rated capacity, causing obese individuals the inability to climb. Obese workers are also at increased risk for sudden incapacitation due to different conditions such as heart attack and stroke, causing confined space entry to be difficult for both themselves and others who would have to rescue the incapacitated person if an emergency occurs. Even if these individuals do not climb, heat stress is 3.5 times more likely to happen in obese than normal weigh individuals because the access weight reduces the body’s ability to dissipate heat, increasing stress on the cardiovascular system.
In our field of wind energy, personal protective equipment (PPE) has a rated capacity, causing obese individuals the inability to climb. Obese workers are also at increased risk for sudden incapacitation due to different conditions such as heart attack and stroke, causing confined space entry to be difficult for both themselves and others who would have to rescue the incapacitated person if an emergency occurs. Even if these individuals do not climb, heat stress is 3.5 times more likely to happen in obese than normal weigh individuals because the access weight reduces the body’s ability to dissipate heat, increasing stress on the cardiovascular system.
Another issue that comes along with obesity is loss productivity. According to Stephanie Pappas, NBC News, “Loss of productivity due to obesity costs as much as medical expenditures for the condition, according to a new study that pegs the cost of obesity among full-time workers in the Unites States at $73.1 billion per year.” This is the equal to hiring 1.8 million new workers with an annual salary of $42,000, essentially losing a tremendous amount of money for organizations.
Researchers have found that obese individuals tend to be less productive than those of normal weight, and a lot of this is linked to sick days. Studies have also shown that lost performance at work doubled with each increase from mild to moderate to extreme obesity (these classifications depend on BMI). The higher the BMI, the higher the impact there is on work productivity. Eighteen percent of the total company cost of obesity is because of lost workdays, and forty-one percent of the extra cost is lost productivity.
For example, research by LAP-BAND found that female employees with a BMI of 30-34.9 had about 6.3 days during a calendar year of lost time while at work. Women, who had a BMI over 40, had an average of 22.7 lost days per year. Men of average weight lost about 2.3 days, versus men whose BMI was over 40 lost an average of 21.9 days.
As of 2012, 34% of the U.S population was of a recommended weight, this percentage is steadily decreasing with a projection of 14% by 2030. This trend can be reversed through a healthy lifestyle that can start today.
Shelby Schneid
Bio: A graduate from Eastern Kentucky University with a B.A. of Public Relations and completing an M.S. of Safety, Security and Emergency Management. All while going to the University of Central Florida pursuing an M.S. of Management concentrating in Human Resources and Change Management. A graduate EHS intern at Siemens Energy in the wind power sector.

Do you have any thoughts? Please share them below